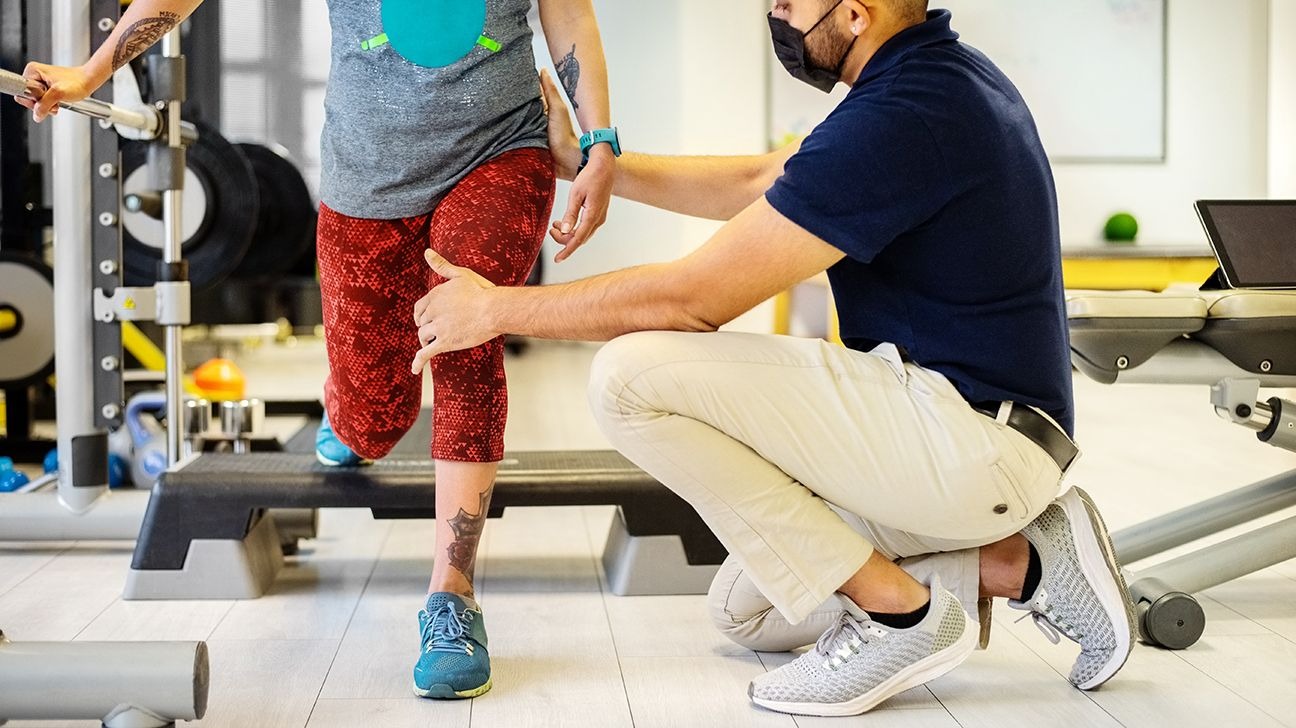
Research following children and adults with cerebral palsy over decades shows a consistent pattern. Function can improve, comfort can increase, and participation in daily life can expand, but change happens gradually and looks different for every person.
Many families arrive at physical therapy with hope mixed with uncertainty, often asking the same question early on. What does physical therapy actually do for cerebral palsy, and what is realistic to expect over time?
Physical therapy is not about fixing cerebral palsy or making it disappear. It is a long term clinical process focused on supporting movement, preventing avoidable complications, and helping each person function as fully and comfortably as possible within their own abilities. This helps patients and caregivers engage with therapy in a grounded and informed way.
The Role of Physical Therapy in Cerebral Palsy

Physical therapy is a key part of cerebral palsy care, but its goals depend on the type of cerebral palsy, severity of movement involvement, and age. A child learning basic motor skills, a teenager managing fatigue and an adult maintaining mobility all require different therapeutic priorities.
Therapy focuses on how the brain injury affects muscle tone, coordination, and movement control. While cerebral palsy itself does not progress, secondary issues such as muscle tightness, joint stiffness, weakness, and inefficient movement can increase over time.
Physical therapy addresses these secondary changes to preserve function and comfort. In some cases, access to therapy is influenced by legal and financial factors. Families affected by preventable birth-related injuries may pursue a cerebral palsy lawsuit to secure long-term support for therapy and care. Physical therapy generally aims to:
- Support functional movement and daily activities
- Prevent secondary musculoskeletal complications
- Improve comfort, endurance, and participation
- Adjust goals across different life stages
What Physical Therapy Aims to Achieve
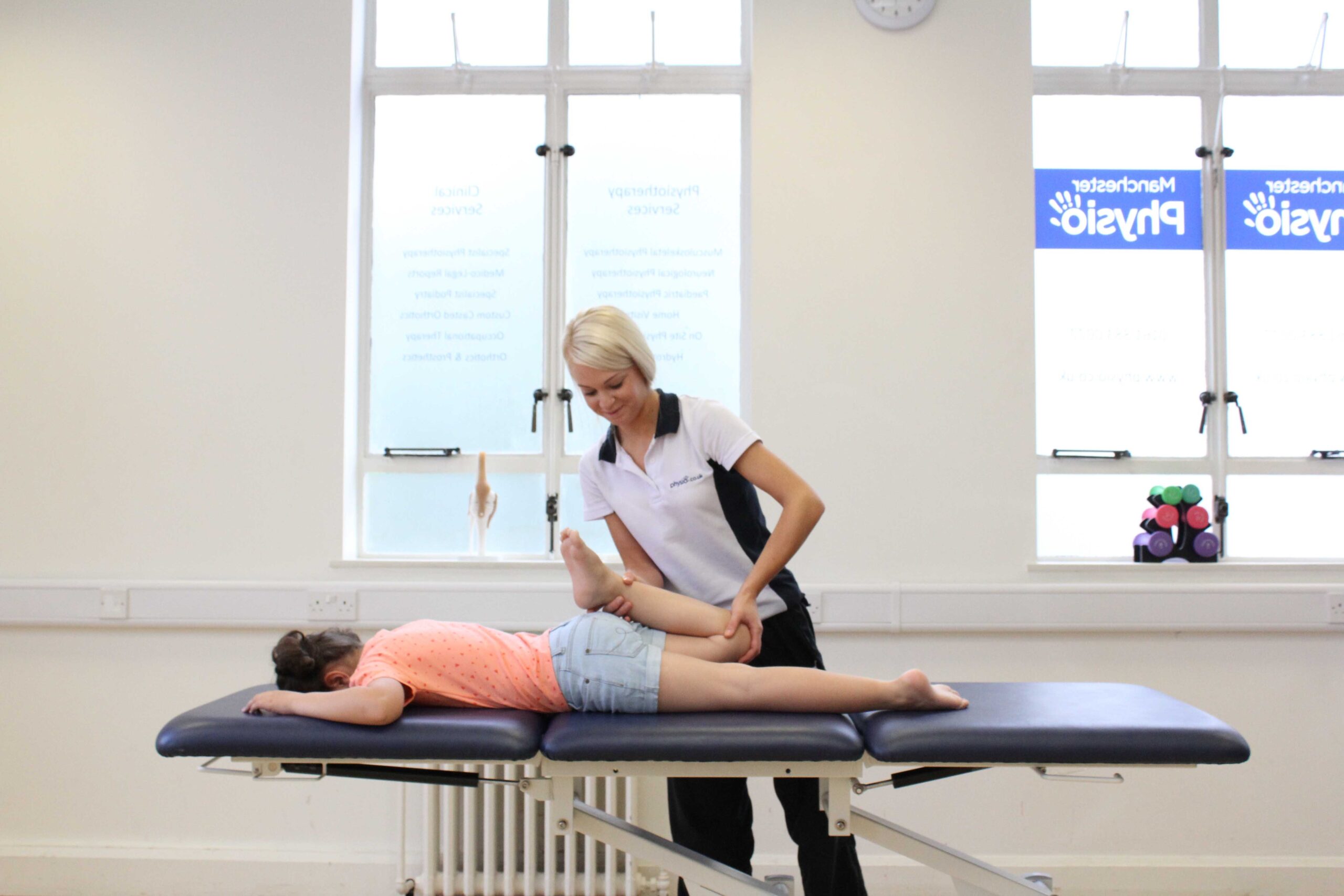
The goals of physical therapy are shaped by functional priorities rather than by a fixed developmental checklist. For some children, therapy aims to support basic mobility such as sitting, standing, or walking with assistance. For others, the focus may be on hand use, balance, or safe transfers.
Adults with cerebral palsy often pursue therapy to manage pain, preserve endurance, and adapt to changes related to aging. Muscle fatigue and joint stress can increase over time, even though the brain injury itself does not worsen.
Before any program is designed, therapists usually consider factors such as functional classification levels, daily environments, and personal goals. These guide realistic planning. Common evidence based goals include the following:
- Supporting functional movement such as rolling, transfers, or gait with aids
- Preventing muscle shortening and joint contractures
- Improving strength and postural control for daily tasks
- Reducing discomfort and improving energy efficiency
- Enhancing participation in school, work, or community life
Progress is measured against these individualized goals rather than against typical developmental milestones.
Common Misconceptions About Physical Therapy and Cerebral Palsy

Many misunderstandings about physical therapy come from unrealistic expectations or outdated beliefs. One of the most common misconceptions is that therapy aims to normalize movement or teach the body to move in a typical way. In reality, therapy works with existing movement patterns, improving safety and efficiency rather than enforcing a specific appearance.
Another misconception is that more therapy always means faster improvement. Intensive therapy can be helpful in certain contexts, but overloading the body may lead to fatigue, pain, or frustration without meaningful benefit. Quality and consistency matter more than volume.
Some families also expect visible progress in every phase of therapy. Plateaus are common and expected; they do not signal failure. It is important to clarify what therapy does not do.
- It does not cure cerebral palsy
- It does not reverse brain injury
- It does not guarantee walking or independence
- It does not follow a universal timeline
Clear communication about these boundaries protects trust between therapists, patients, and families.
Types of Exercises Used in Therapy and Their Purpose

Physical therapy exercises are chosen for their functional purpose rather than for repetition alone. Each activity supports a specific aspect of movement or daily participation. Programs are adjusted frequently based on response and tolerance.
Therapists may include activities that focus on mobility, such as assisted transitions between positions or supported walking. Strengthening exercises aim to improve muscle activation and endurance rather than bulk. Balance activities help with stability during standing or reaching.
Postural work addresses trunk control and alignment, which affects breathing, feeding, and hand use. Functional skill practice may include stair negotiation, transfers, or wheelchair mobility depending on individual needs.
Any exercises suggested outside of therapy sessions are typically provided as guided examples under professional supervision. They are adapted carefully to avoid injury or overuse. The value of these exercises lies in how they translate into daily life, not in how many repetitions are completed.
How Progress is Evaluated in Clinical Practice
Progress in cerebral palsy therapy is evaluated using functional and practical markers rather than isolated muscle measurements. Therapists look at how movement changes affect daily activities, comfort, and participation.
Formal assessment tools may be used periodically, but much of the evaluation happens through observation and discussion. Families often notice changes before numbers shift on a scale.
A therapist may track progress in areas such as endurance during walking, ease of transfers, or reduced need for assistance. Comfort during sitting or sleep can also be a meaningful marker. Evaluation often includes:
- Changes in functional ability during daily routines
- Improved tolerance for activity or positioning
- Reduced pain or muscle stiffness
- Greater independence with assistive devices
- Increased participation in social or educational settings
Progress may be subtle. A task becoming less tiring or less painful still represents real clinical improvement.
What Progress Typically Looks Like Over Time

Progress in physical therapy for cerebral palsy rarely follows a straight upward line. Gains often occur in phases, with periods of visible improvement followed by stabilization. Growth spurts, illness, or life transitions can temporarily affect function.
In children, progress may align with developmental stages, but at an individual pace. In adults, therapy often focuses on maintaining skills and adapting strategies as physical demands change. It is common for goals to evolve over time. Early therapy may prioritize mobility, while later phases emphasize endurance, joint protection, or pain management.
Did you know: Loss of function in adulthood is often linked to untreated muscle tightness and fatigue rather than to cerebral palsy itself. Ongoing therapy can help reduce this risk.
Understanding progress as adaptation rather than constant improvement helps set realistic expectations and supports long term engagement with therapy.
Emotional and Practical Expectations for Families and Patients
Families and individuals living with cerebral palsy often carry emotional weight alongside physical challenges. Slow progress can feel discouraging, especially when effort is high and change is gradual. Acknowledging this experience is part of responsible care.
Therapy works best when integrated into daily life without becoming overwhelming. Collaboration between therapists, physicians, educators, and caregivers supports consistency and reduces conflicting advice.
Practical expectations include the need for long term involvement, periodic reassessment, and flexibility in goals. Therapy intensity may change across life stages.
Blockquote: Cerebral palsy is a lifelong condition, but functional needs and priorities evolve. Physical therapy adapts alongside these changes rather than aiming for a final endpoint.
Supportive communication and realistic planning help families stay engaged without feeling pressured to meet external benchmarks.
Long Term Outlook and Realistic Expectations

Physical therapy for cerebral palsy is a long term, adaptive process focused on supporting movement, comfort, and participation over time. Outcomes vary widely based on individual needs, health, and access to care, with no fixed timelines or universal milestones.
Progress is often seen in practical ways such as easier daily activities, reduced discomfort, or improved confidence in movement. When therapy is evidence based and guided by licensed professionals, it provides ongoing support rather than a promise of dramatic change. The goal is to maintain function, limit secondary complications, and support quality of life in a way that respects the lifelong and variable nature of cerebral palsy.